One question we commonly get asked is how birth control may impact HPV. Birth control is commonly used by women of reproductive age to prevent pregnancy. Today, many also use birth control to support hormonal symptoms like PMS, acne, dysmenorrhea, and heavy menstrual bleeding.
Many factors are often considered when choosing a birth control that is right for you. In this article, we will explore three popular birth control methods and things to consider with regard to HPV.
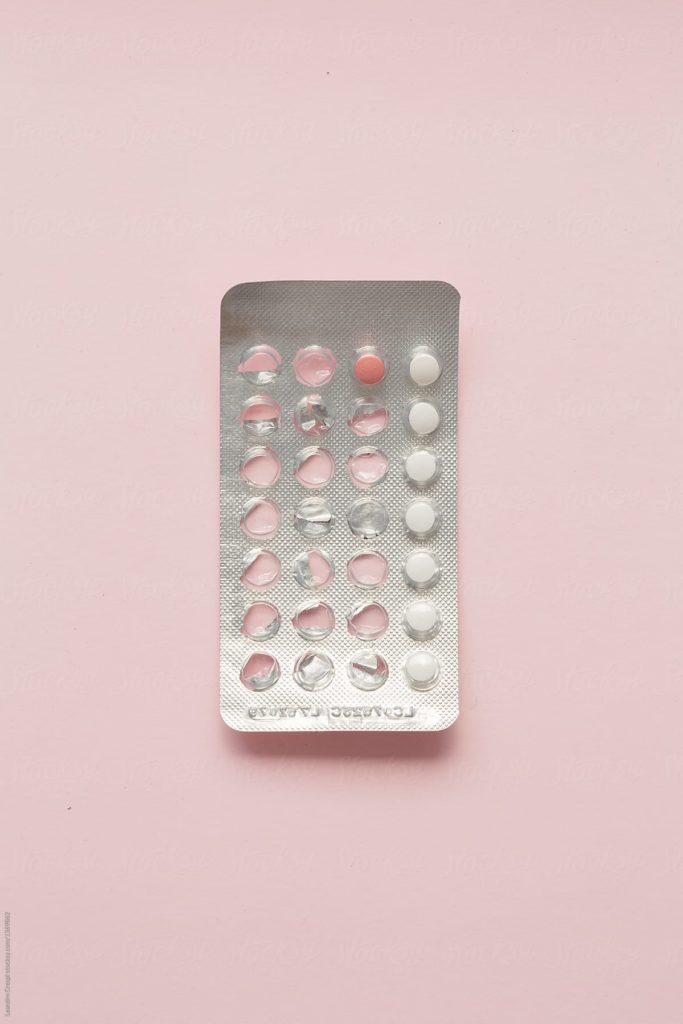
Let’s Start With The Oral Contraceptive Pill (OCP)
The OCP is a hormone modulating birth control. The OCP contains estrogen and progesterone, two hormones involved in the reproductive cycle. Individuals who menstruate often go on the OCP to prevent pregnancy as well as control hormonal symptoms like premenstrual syndrome (PMS), acne, painful periods, and heavy menstruation.
The OCP is speculated to increase HPV persistence and progression. The pill may do this by altering certain genes as well as increasing the cervical maturation process which allows cell proliferation of HPV. By taking a synthetic hormone you may change the susceptibility of the cervical cells to high-risk infections. Moreover, because the OCP contains growth-stimulating hormones estrogen and progesterone, there is some risk that they can increase the risk of cervical cancer.
Studies have found that long-term use (10 years or longer) of oral contraceptives has a four-fold increased risk of developing cervical cancer. A study of over 46,000 individuals found that those who are used OCP had a significantly higher rate of cervical cancer and abnormal cervical cell growth than non-users. The research does also suggests that the risk decreases after stopping the pill. HPV rates decline with time since quitting.
The OCP may also lead to nutrient deficiencies associated with HPV. The pill can deplete riboflavin, vitamin B6, folic acid, vitamin C, and zinc. We know these nutrients are important players in supporting the immune system and some have even been specifically linked to HPV.
Moreover, the birth control pill is also known to alter the gut microbiome. The pill may increase leaky gut, dysbiosis, and candida overgrowth. A healthy gut is another foundation for our immune and overall health. Impairing this system can have a widespread impact on the rest of the body.
Considering these impacts, it is important to support nutrient levels and gut health if taking the OCP. We recommend optimizing dietary intake of diverse fruits and vegetables, fibers, and probiotic foods as well as considering supplementation.
Condoms
Condoms are a favorable form of birth control when it comes to protecting against Sexually Transmitted Infections (STIs) and pregnancy. Condoms form a barrier between mucosal contacts and are found to be 98 percent effective at protecting against STIs like chlamydia and gonorrhea. However, because skin-to-skin contact can still occur with condom use, they are less effective at preventing the spread of herpes, genital warts, and HPV.
That’s right. Unfortunately, HPV can still be transmitted through condom use.
Nevertheless, condom use is still warranted and recommended. Some studies have found that the risk for genital warts and the grade of cervical intraepithelial neoplasia (CIN) was reduced in condom users. Condoms also protect against other STIs and infections that can contribute to co-infections and impair the vaginal microbiome.

IUD
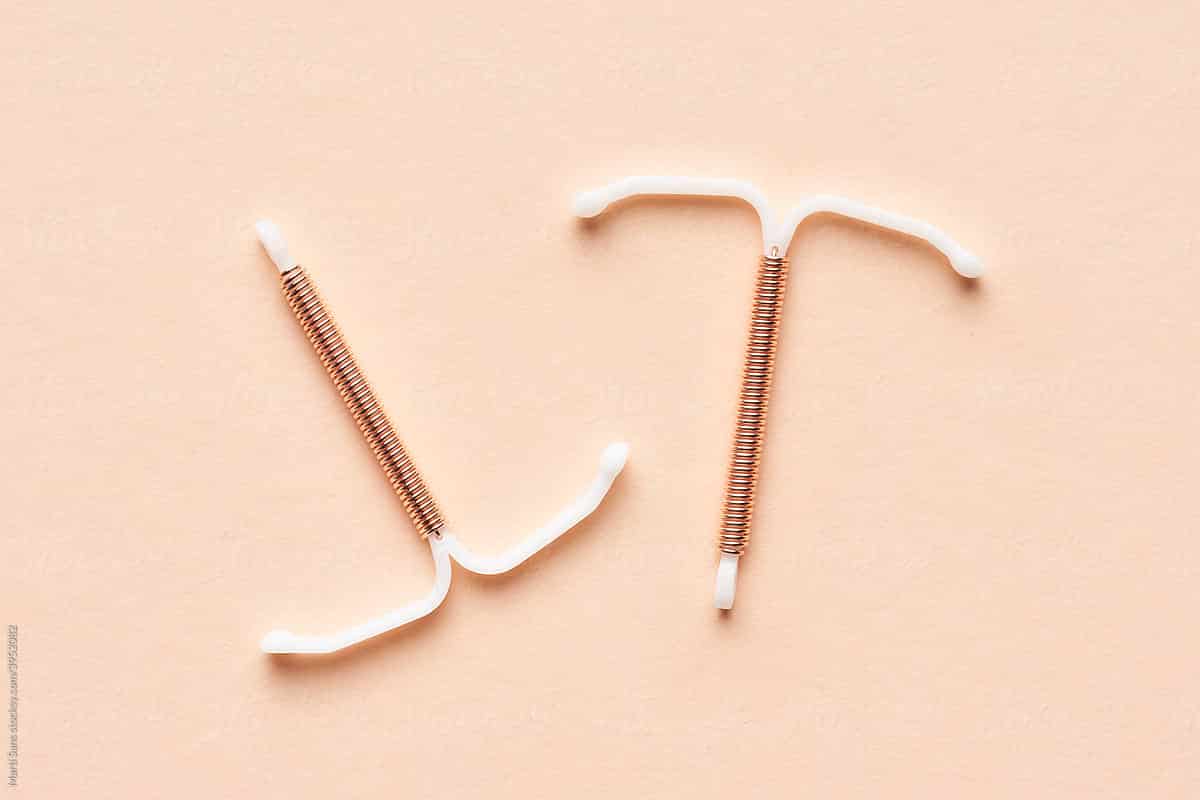
The intrauterine device comes in both a hormonal and non-hormonal form. Both are inserted into the uterus for long-term, effective pregnancy prevention.
The hormonal IUD delivers a small amount of progestin to the local uterine tissue. Some individuals notice side effects like changes in mood, bloating, cramping, or reduced menstruation. The IUD can also get displaced and in rare cases perforate the uterus.
The hormonal release of the IUD is lower than the OCP. The IUD releases one hormone, progestin, at a dose of fewer than 20 micrograms each day. Whereas the OCP releases 1 milligram of progestin and 0.02 to 0.06 milligrams of estrogen each day.
The non-hormonal option is a copper IUD that prevents pregnancy by releasing copper in the uterus that is toxic to sperm. The copper IUD will not suppress ovulation and the most common side effect is heavier menstrual bleeding. While the copper IUD has no hormonal impact, the heavier menstrual bleeding can contribute to iron deficiencies and anemia.
What’s The IUD Connection with HPV?
Some studies have shown that sexually active individuals with the IUD group had higher clearance rates of HPV. While others, when adjusted for other variables, found no association between IUD use and HPV infection or persistence.
Research comparing the difference between the copper IUD and hormonal has found mixed results. One study found the hormonal IUD to have a lower risk of high-risk HPV than the copper IUD. Another study found the copper IUD to have a lower risk of cervical neoplasm. Overall, it is unclear how these devices are influencing cervical dysplasia and HPV infections or the mechanism of action.
It is also important to note that the IUD and OCP do also not protect against other STI’s like chlamydia and gonorrhea, while condoms do.
So how can you decrease your risk of HPV?
You are probably thinking, what then can I use to protect myself against HPV and STI’s? Currently, condoms and engaging with fewer sexual partners are the best ways to reduce your risk of exposure to HPV. However, we understand that other factors are involved. We always recommend talking to your health practitioner to help decide what is best for you.
Because most sexually active individuals carry some form of HPV and it can be transmitted through skin contact, no form of birth control can completely protect you.
More importantly, you can support your whole-body system so that if you are infected, you are better equipped to defend against pathogens and viruses.